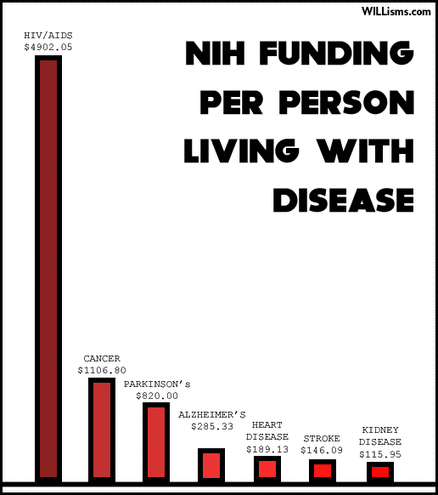
 At less than $5 per person, ME/CFS is somewhere below the black line.
At less than $5 per person, ME/CFS is somewhere below the black line. "To make significant progress," the letter said, "funding needs to be provided on par with that of other diseases that are similarly prevalent and disabling."
In order to do all the things the P2P panel has recommended in its Report, more funding is needed. But not only did the Draft Report fail to include amounts for future NIH research, it suggested funding avenues that were entirely inadequate for meeting current research needs.
The IACFS/ME letter also made a point of recommending that ME/CFS be moved from the Office for Research on Women’s Health (ORWH) to an Institute that actually has funds.
"We respectfully suggest either NINDS or NIAID as the primary Institute as multiple studies demonstrate that neurologic, infectious, and autoimmune components are present in this illness."
Nothing has been more detrimental to ME/CFS research grants than its current location under the auspices of ORWH. Back in the 1980s, when CFS was considered a contagious illness, it was represented by NIAID (National Institute of Allergy and Infectious Diseases). Funding, at that time, was devoted mainly to investigating viral etiology, but other biomedical research was pursued as well. Once CFS was moved to the ORWH, funding for serious biomedical research all but vanished.
The IACFS/ME's suggestion to house ME in the National Institute of Neurological Disorders and Stroke (NINDS), which has a budget of $1.5 billion, or NIAID, with its budget of over $4.4 billion makes perfect sense - provided that the NIH has more than a token interest in advancing research into the causes, mechanisms, and treatment of ME/CFS.
____________________
Dear NIH P2P Panel Members,
As board members of the International Association for Chronic Fatigue Syndrome/ Myalgic Encephalomyelitis (IACFS/ME), the largest international group of clinicians, researchers, and other professionals dedicated to the care and research of patients with ME/CFS, we hope that your report will have a positive influence on the field, our organization’s members, and the patients/ families we serve.
Generally we agree with the majority of the Panel’s recommendations but believe that the elephant in the room – research funding – alluded to in the report (e.g. Line 8) needs to be addressed more strongly and specifically. Federal funding for ME/CFS research over the last 3 decades has been inadequate to the broad-ranging and complex challenges presented by this illness. In recent years, only $5-$6 million annually has been awarded on an extramural basis, resulting in ME/CFS being the least-funded out of 240+ conditions that NIH tracks annually.
(http://report.nih.gov/categorical_spending.aspx) Over the last 25 years that IACFS/ME has been in existence, we have seen few new researchers enter the field, a flat publication rate over the past decade, and continuing stigma surrounding the illness.
This state of affairs is particularly concerning given the costs to society of this illness with respect to lost productivity and high health care costs. To whom do the one million US patients with ME/CFS turn to be reassured that their illness is being taken seriously with substantive commitments to scientific research? Only the federal government, and NIH in particular, has the ability to make such commitments.
Many of the same recommendations and concerns highlighted by the Panel have been brought up by members of our organization over the years. For example, last Spring, several of our board members who also served on DHHS’ CFS Advisory Committee suggested that NIH establish and support a data/ biobank-sharing platform and/or issue a Request for Applications focusing on specific areas to jumpstart research. Unfortunately, the recommendations were not accepted or acted upon by NIH. (http://www.hhs.gov/advcomcfs/recommendations/hhs-cfsac-recommendations-response.pdf)
The reasons given were that there were too few ME/CFS researchers to invest the funds for such a platform, that such funding would take away money from other ME/CFS projects, and that since so little was known about ME/CFS, a RFA was not the right mechanism for funding. Interestingly, the letter then went on to state “RFAs are designed to build upon recommendations that have been identified……. [through] workshops and conferences” yet no RFA was issued for ME/CFS after NIH’s State-of-the-Knowledge Workshop on ME/CFS in 2011 despite the efforts of then-Trans-NIH-Working-Group head Dr. Dennis Mangan. The letter concludes by suggesting that mentored career development, student, and post-doctoral training grants be used.
(The last time NIH issued and RFA for ME/CFS, in 2007, a number of successful projects were funded.) (http://www.hhs.gov/advcomcfs/recommendations/06142014.html)
The essential message conveyed is that the US government does not want to invest additional funds because not enough is known about the disease and there are not enough researchers. Yet a critical reason why we have a dearth of researchers and knowledge is because of the poor funding situation, which has endured for the past 3 decades. Lack of investment in basic research by the government also impacts other sources of ME/CFS research funding. In April of 2013, the US Food and Drug Administration hosted a Drug Development workshop for ME/CFS. The pharmaceutical representatives who attended cited poor understanding of the basic pathophysiology of ME/CFS as a major reason for the reluctance of their companies to invest in ME/CFS clinical research.
Finally, we believe it would be beneficial to change the institutional affiliation of ME/CFS from the Office for Research on Women’s Health (ORWH) to an Institute with research funds to distribute. ME/CFS may have been placed under ORWH originally so that funding could be coordinated across institutes but that has not been successful. In fact, the Program Announcement for ME/CFS includes an October 2014 note that several Institutes – including NIA, NIDDK, NIEHS, and NCCAM – have withdrawn their participation. (http://grants.nih.gov/grants/guide/pa-files/PAR-12-032.html)
Thus we encourage the NIH to consider assigning the management of CFS/ME research to a single NIH Institute and provide that Institute with the responsibility and appropriate funding to effectively manage the research effort in this disease. We respectfully suggest either NINDS or NIAID as the primary Institute as multiple studies demonstrate that neurologic, infectious, and autoimmune components are present in this illness. To make significant progress, funding needs to be provided on par with that of other diseases that are similarly prevalent and disabling. For example, multiple sclerosis and systemic lupus erythematosus are both funded at more than ten times the level ($112-$152 million and $92-$127 million annually respectively) of ME/CFS although ME/CFS, even using a conservative estimate, may be more common.
Thus we respectfully ask that the NIH Panel highlight the inadequate research funding of ME/CFS and link this core premise to specific recommendations for new funding initiatives, with dollar amounts, mechanisms, and deadlines, to begin to address the current underfunded status of this illness.
We also agree with the Panel’s suggestion that carefully constructed and operationalized case definitions are needed for research but disagree that the main issue is lack of agreement on a single research case definition. A single case definition, the 1994 Fukuda case definition, has been used for the majority of the studies worldwide. However, there are concerns that Fukuda is neither sensitive nor specific enough to capture the patient population it is meant to capture; furthermore, it has not been updated in 20 years to reflect clinician/ patient experience, substantial new evidence from more recent studies on symptom frequencies, and newer case definitions in ME/CFS.
Thus, we ask that the Panel instead emphasize that any research case definition used be based on clinician/ patient experience and the scientific literature, be operationalized well enough that it is easily duplicated across studies by different researchers, and that it be validated and reassessed in a timely manner.
Thank you for this opportunity to comment on the Draft Executive Summary. We hope that you will take our suggestions into account and will feel no hesitation in contacting us if we can be of further service.
Sincerely,
Fred Friedberg, Ph.D.
President, IACFS/ME
Staci R Stevens, M.A.
Founder: Workwell Foundation; Ripon, CA
Co-Vice President, IACFS/ME
Rosamund Vallings, MNZM, MBBS
Howick Health and Medical Center; Auckland, New Zealand
Secretary, IACFS/ME
Julia Newton, MD, PhD
Dean of Clinical Medicine & Professor of Ageing and Medicine
Clinical Academic Office, The Medical School, Newcastle University; New Castle upon Tyne,
United Kingdom
Board member, IACFS/ME
Jon D. Kaiser, MD
Clinical Faculty, Dept. of Medicine, UCSF Medical School; San Francisco, CA
Medical Director, K-PAX Pharmaceuticals, Inc.
Board Member, IACFS/ME
Steven P. Krafchick MPH, JD
Krafchick Law Firm PLLC, Legal Services for Injured and Disabled People; Seattle, WA
Board member, IACFS/ME

 RSS Feed
RSS Feed
